Getty Equipment used to test for high blood pressure.
The risks associated with COVID-19 don’t increase if you’re taking blood pressure medication, according to two research studies.
The research studies looked at two different types of blood pressure medication, ACE inhibitors (drugs ending in -pril) and ARBS (drugs ending in -sartan). Some of the brand names are lisinopril, captopril, losartan, valsatan, zestril, prinicil, cozaar and atacand.
Hypertension is a widespread problem in the United States, where estimates say one in three Americans suffers from high blood pressure severe enough to need medication.
Here’s what you need to know:
One Study Found ‘No Substantial Increase’ in Risk of Getting COVID-19 or in Getting Severe COVID-19 if Infected
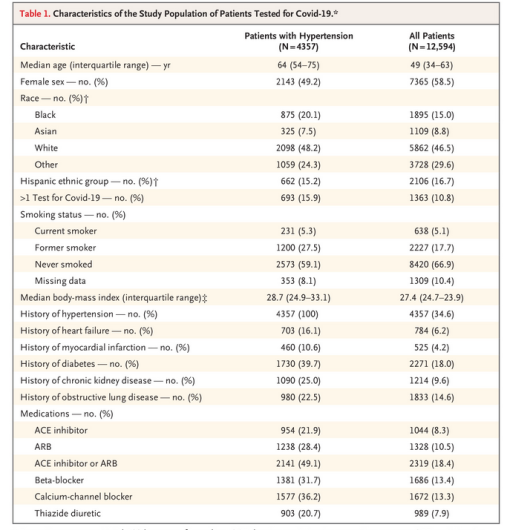
A table from the study
The first study in question is called Renin–Angiotensin–Aldosterone System Inhibitors and Risk of Covid-19 and was published in the New England Journal of Medicine. It was released on May 1, 2020.
The researchers wrote:
We assessed the relation between previous treatment with ACE inhibitors, angiotensin-receptor blockers, beta-blockers, calcium-channel blockers, or thiazide diuretics and the likelihood of a positive or negative result on Covid-19 testing as well as the likelihood of severe illness (defined as intensive care, mechanical ventilation, or death) among patients who tested positive.
They studied more than 12,000 patients.
Among 12,594 patients who were tested for Covid-19, a total of 5894 (46.8%) were positive; 1002 of these patients (17.0%) had severe illness. A history of hypertension was present in 4357 patients (34.6%), among whom 2573 (59.1%) had a positive test; 634 of these patients (24.6%) had severe illness. There was no association between any single medication class and an increased likelihood of a positive test. None of the medications examined was associated with a substantial increase in the risk of severe illness among patients who tested positive.
The study concluded: “We found no substantial increase in the likelihood of a positive test for Covid-19 or in the risk of severe Covid-19 among patients who tested positive in association with five common classes of antihypertensive medications.”
This study looked at patients “in the New York University (NYU) Langone Health electronic health record.”
The Second Study Found That There Was No Difference in Severity, Complications or Risk of COVID-19 for Patients on Some High Blood Pressure Medications
GettyThis photo from the Centers for Disease Control and Prevention (CDC) shows a microscopic view of the Coronavirus.
The second study was called Association of Renin-Angiotensin System Inhibitors With Severity or Risk of Death in Patients With Hypertension Hospitalized for Coronavirus Disease 2019 (COVID-19) Infection in Wuhan, China. It was published in late April 2020 in JAMA Cardiology journal.
This study sought to answer the question:
Among patients with hypertension, do those taking angiotensin-converting enzyme inhibitors (ACEIs) or angiotensin receptor blockers (ARBs) have greater illness severity or increased risk of mortality during hospitalization for coronavirus disease 2019 (COVID-19) infection?
The study involved “362 patients with hypertension hospitalized with COVID-19 infection.”
Its conclusion? “There was no difference in severity of the disease, complications, and risk of death in those who were taking ACEIs/ARBs compared with those not treated with these medications.”
The researchers added, “In this single-center study, ACEI/ARB was not associated with severity and outcomes of COVID-19 infection in hospitalized patients with hypertension. These results support current guidelines and societal recommendations for treating hypertension.”
According to The New York Times, there are also studies under way looking at whether high blood pressure medications reduce the risk of COVID-19.
Medical groups have not suggested that people discontinue high blood pressure medications during the pandemic.
The American College of Cardiology previously released a statement advising that “Currently there are no experimental or clinical data demonstrating beneficial or adverse outcomes with background use of ACE inhibitors, ARBs or other RAAS antagonists in COVID-19 or among COVID-19 patients with a history of cardiovascular disease treated with such agents.”
The organization noted that the HFSA, ACC, and AHA “recommend continuation of RAAS antagonists for those patients who are currently prescribed such agents for indications for which these agents are known to be beneficial, such as heart failure, hypertension, or ischemic heart disease.”
READ NEXT: Is a Sore Throat an Early Symptom of Coronavirus?